Understanding Functional Gastrointestinal Disorders (FGID)
Published on 30th August, 2021

Understanding Functional Gastrointestinal Disorders
Functional Gastrointestinal Disorders (FGID) are a group of disorders characterized by chronic GI symptoms such as abdominal pain, dysphagia, dyspepsia, diarrhea, constipation and bloating. They occur due to abnormal functioning of the GI tract but have an absence of pathology during testing (i.e., no indications of biochemical abnormalities, no growth of tumors or masses).
Features of FGID
FGIDs are known to be brain-gut interaction disorders as there is disharmony noted between the brain and GI communication. In FGID, the muscular activity of the GI tract (motility) is abnormal, where there is presence of muscular spasms that cause pain. In addition, the nerves of the GI tract are highly sensitive (sensation) that normal contractions, such as digesting a meal, can cause discomfort. Overall, FGIDs have a significant negative impact on an individual’s quality of life, health care costs and work productivity.
Factors affecting FGID
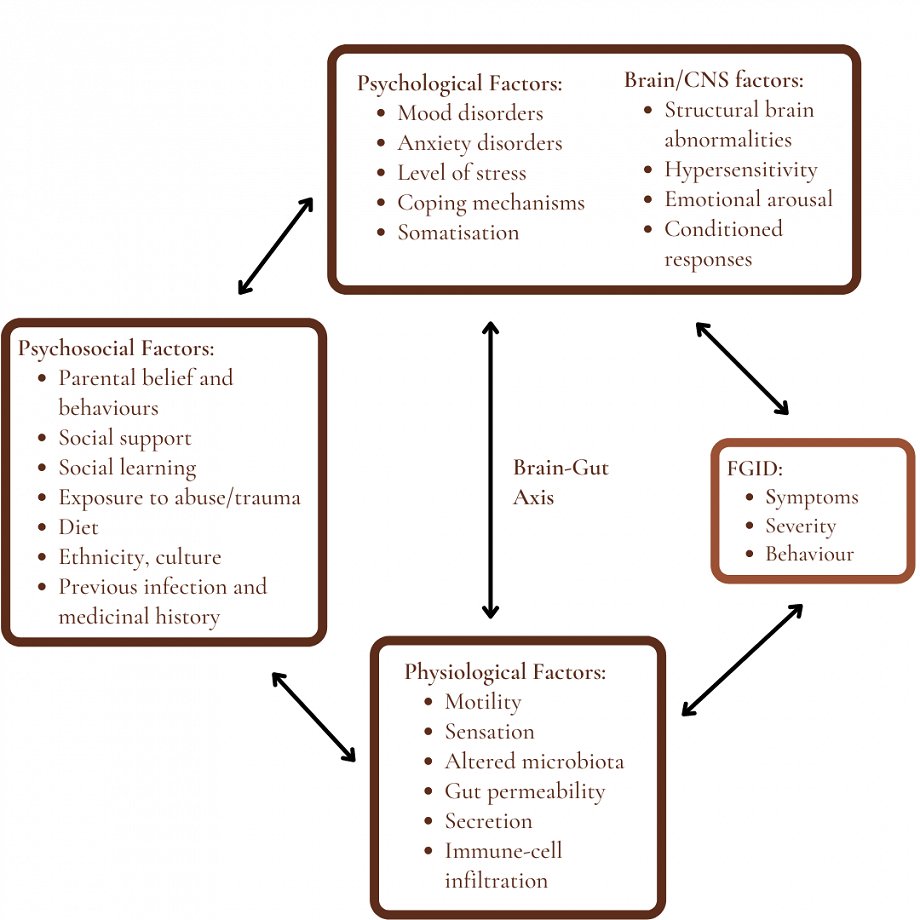
External stressors, emotions and thoughts can affect GI features. As there is bi-directional pathway between the brain and the GI tract, activity in the gut can also affect pain perception, mood and behaviour. Psychosocial disturbances can also increase and modulate the experience of FGIDs and health outcomes.
Management and treatment of FGIDs
The aim of management is to provide individuals with more control over their symptoms so that it does not govern their life. In management, a biopsychosocial perspective is employed in identifying factors that trigger or maintain the symptoms and focusing on altering these factors. An integrated and multidisciplinary approach is taken to facilitate management of individuals’ treatment needs.
Tips to help with management
1) Improving lifestyle
Stress and fluctuations with mood have been associated with pain intensity. Adequate amount of sleep and regular exercise routine helps with both the factors and FGID symptoms. Physical activity has been shown to reduce severity of Irritable Bowel Syndrome (IBS; a type of FGID). It also has been proven to reduce stress, elevate mood and help with quality of sleep.
Even a simple exercise such as walking done for about 20 minutes (3-5 times per week) helps with management of FGID symptoms and pain.
2) Diet and Nutrition
Caffeine and alcohol are known to contribute to disrupted sleep and have been associated with FGID symptoms such as diarrhea and reflex symptoms. Minimizing intake of these and avoiding them during late evenings may help with some of the symptoms.
As food intake is associated with FGID, keeping a food diary can help identify foods that trigger symptoms to be avoided in the future. Reducing intake of lactose, high-starch and sugary food and drinks have also been proven to help with symptom management.
Treatment of FGID
As mentioned earlier, FGID treatment is multi-disciplinary and can involve physicians, dieticians and psychologists. Hence, symptoms may also be treated pharmacologically where deemed necessary. Assessing individual’s quality of life and psychological well-bring, they may also be advised to attend therapy sessions with psychologist. Therapy aims would include managing their worries and maladaptive thoughts stemming from pain associated with FGID.


