Depression and Anxiety - it is not just in your head but may be a Central Nervous System Response
Published on 28th July, 2020 by Dr. Sanveen Kang

Over the years, I have found time and time again that the mind and the body function very much together. This would not come as a surprise to many of us. However, this view is integrated only to a small degree when treating mental health disorders. Contrary to popular belief, mental health conditions across the lifespan may be due to an underlying sensory processing disorder.
A brief overview on Sensory Processing and Mental Health
Clinicians and researchers have long grappled with the challenge of categorizing, describing, and understanding mental disorders, with imperfect results. Mental health symptoms are complex and dimensional in nature; making it a very perplexing task to simplify these experiences in simple categories.
Jagiellowicz and colleagues (2010) along with Aron and colleagues (2012) stated that sensory processing sensitivity (SPS) is defined as a genetically determined personality trait described by “social, emotional, and physical sensitivity”. As studied by Jagiellowicz et al. (2010), variation in this trait is associated with neurobiological differences. Jagiellowicz et al. (2016) demonstrated the link between those high in SPS and greater activation of brain regions involved in high-order visual processing when images with subtler alterations were shown. Acevedo et al. (2014) found a positive correlation between higher SPS, and activation of brain regions involved in attention, empathy, and action planning. SPS has been shown to have overlapping features with sensory processing abnormalities present in range of disorders such as ASD, schizophrenia, mood disorders and post-traumatic stress disorder (PTSD). Research has also shown that mental health disorders impact sensory perception and vice versa.
It is important to recognize that sensory sensitivity would be one part of the overarching concept of Sensory Processing Disorder (SPD). However, SPD is not listed in the current edition of the Diagnostic and Statistical Manual of Mental Disorders, 5th Edition: DSM-5 (2013). Instead, the DSM-5 includes sensory concerns as criteria for Autism. It is also important to note that not everyone with Autism has sensory processing disorder.
Did you know that many “neuro-typical” individuals experience difficulties processing sensory information too?
The sensory system is a part of the Central Nervous System (CNS). Therefore, it is safe to assume that it affects many domains of its functioning including the Autonomous Nervous System (ANS). Affective processing also activates the ANS. More specifically, Anxiety activates the ANS whilst autonomic function affects risk depression.
So, what does this mean for yourself and/or your child?
Let’s take the example of anxiety. For many people with SPD, anxiety comes as part of the package. SPD and anxiety work together to cause mayhem. They play off each other, and create a spiral effect of symptoms.
When you or your child has anxiety from sensory issues, it presents itself the same way non-sensory anxiety does; the symptoms are virtually the same. It can be hard to distinguish between sensory overload and anxiety. Most commonly, SPD anxiety can look like this and mimic a freeze response:
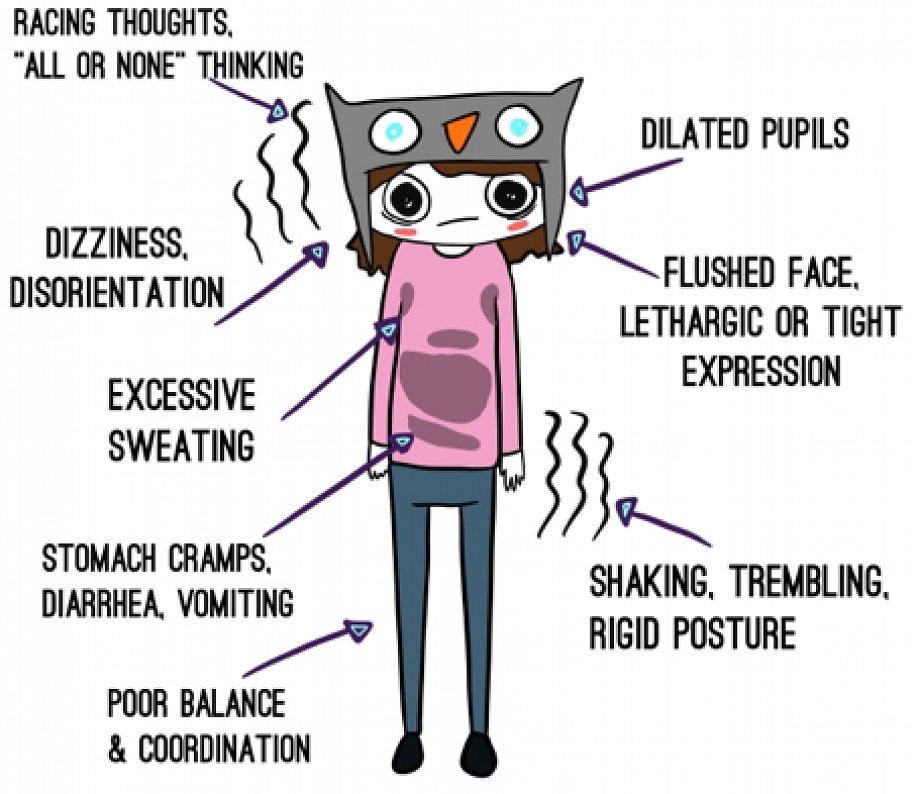
In my work with clients, I have also found that incorporating sensory processing into psychological therapy helps with regulating emotions and behavior (through the understanding and incorporation of the role of the sensory systems in processing information from the body and environment). As a result, clients (children, teens and adults) appear to be more receptive to psychological input and treatment outcomes appear to be reached much quicker. Improvement in daily functioning, especially in terms of the ability to focus, concentrate and be ready for engagement in the task at hand, have also been observed. Therefore, a sensory room or materials and sensory-based treatment has positive outcomes.
Here are some sensory-based strategies you may wish to try yourself or with your child:
1. For anxiety, first start by understanding anxiety. Then consider the following strategies to assist with relaxing and calming down.
- Enroll in activities that are likely to reduce anxiety. These are likely to be ones that involve heavy muscle work and muscle stretch (proprioception) (e.g. martial arts, dance, rock climbing, gymnastics, daily chores etc.). Use your best judgement about what is safe and appropriate for your child.
- Try muscle squeezes. Tense the whole body like a rock and hold the position for 10 seconds. Then release with “no muscles”. Repeat this technique three times. Follow with hand clenches. Squeeze the hands into fists and hold them for 10 seconds. Release and repeat three times
- Snuggle under heavy blanket
- Roll back and forth on a yoga ball
- Jump on a trampoline
- Blow up a balloon
- Deep belly breaths and blowing out through “duck lips”
- Use calming scents
- Suck on a lollipop
- Use a tactile fidget toy or sensory touch bar for desks
2. For depression, there would be overlaps with the strategies included above – proprioceptive work and breathing exercises. On top of sensory strategies, we can also add environmental strategies. Here are examples:
- Balancing daily schedule - A good mix of rest, play/ leisure and productivity. Starting out the day with a familiar or preferred activity
- Monitoring demands
- Visual schedules
- Breaking down tasks into simpler steps and supporting the individual as they perform a meaningful activity
- Create a low stress home environment
- Create opportunities for success by enabling child's strengths through play, daily chores, homework and social interaction
- Help your child create a morning routine that is of a pace that suits the child in preparation for the day - extra time to participate in daily activities
- Focus on activities of preference and interest
- Raise awareness of child's performance difficulties to school teachers to create a more positive learning environment and experience for the child
- Raise awareness to teachers for example, of child's emotions and mood that may be side-effects of medication or symptoms
To learn more about SPD Read more on Sensory Integration
Remember to look for your child’s response during and after each activity. Do they appear calm or relaxed?
Should you be keen to learn more about Sensory-Based Treatment Approaches for Anxiety and Depression, contact us at Psych Connect for a chat. At Psych Connect, we are committed to providing therapy without barriers to our clients and are always developing new approaches to reach positive outcomes. When engaging in Sensory-Based Treatment Approaches, our mental health team collaborates with our occupational therapists; embodying the TAC approach to treatment (Team Around a Child).



