Cognitive Behavior Therapy - What is CBT?
Published on 26th June, 2021 by Dr. Sanveen Kang
What is CBT?
Cognitive Behavioural Therapy (CBT) is a form of psychological treatment that focuses on identifying and changing thought patterns that have a negative influence on behaviour and emotions. CBT is considered to be a gold standard treatment approach.
CBT is based on principles that assume that we face difficulties psychologically due to our unhelpful ways of thinking, unhelpful behaviour that we have learned over time, and that we are able to replace these unhelpful ways with helpful ones which helps us cope better with our issues.
How does it help?
CBT focuses on a person’s present, rather than the past that may have led to them developing their difficulties. CBT posits that each of us have a core belief about ourselves, that we develop through our life experiences. Core beliefs are our thoughts about ourselves, others and the world that determine how we interpret our interactions and gain meaning from our experiences. For example, someone who has been abused since childhood, could develop core beliefs that they are not worthy of love or that no-one cannot be trusted. Such beliefs would then automatically activate negative thoughts when said person is placed in a difficult situation. Negative thoughts lead to negative emotions and unhelpful behavior/actions.
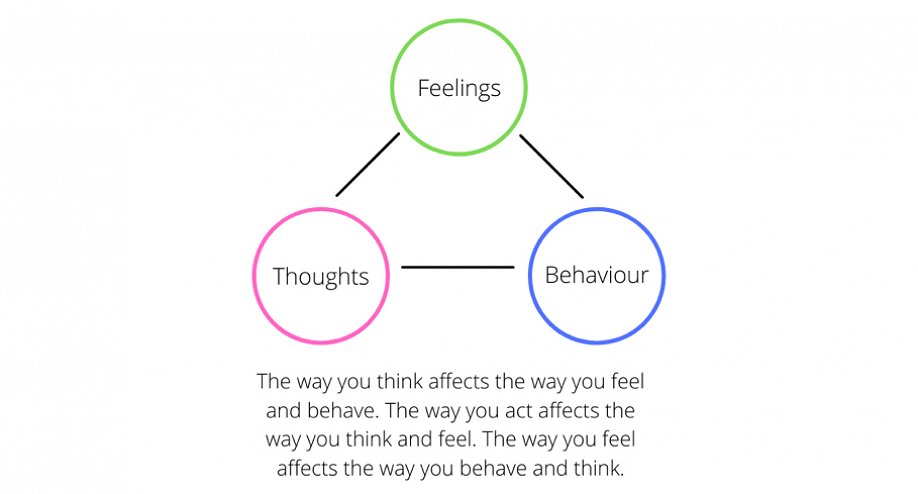
During CBT sessions, you would identify distortions in your thinking, be challenged to eventually replace these negative thoughts with realistic and objective ones. By being able to reframe your thoughts positively or realistically, you influence your emotions and consequently, your behaviour.
CBT aims to allow the person to be self-sufficient by learning how to recognise the faults in their thinking, providing them the tools necessary to problem solve in difficult situations and gain a better sense of confidence in their own abilities.

How does it differ across different age groups?
CBT has been shown to be effective in treating various mental health conditions and across different age groups. Studies have shown that receiving CBT has significant reduced symptoms for children and adolescents with Anxiety disorders, and for adolescents with ADHD .
Across the different age groups, the delivery of CBT may differ depending on their level of understanding. However, the concepts and principles that CBT is based on does not change and remains intact. All clients, regardless of age, would be introduced to CBT along with a description of what they can expect and what is expected of them during the sessions.
As a goal-oriented treatment, there would be focus on resolving problems faced by the client presently and steps to achieve goals. This would mean “homework” assignments for clients to apply the skills, taught during sessions, in settings outside of therapy sessions or clinic (i.e., home, workplace and school). Hence for children and adolescents, parents are asked to be involved in the process to help when necessary. While for adults, CBT is a predominantly verbal process, this may differ for children and adolescents. Simplified explanations, metaphors and visual aids would be incorporated into the approach for children and adolescents.
Characterizations or imaginative role play such as being a superhero, renaming skills as super powers or visualizing anxiety as a gremlin, could be used to help children understand the abstract concepts and learn the necessary skills. Homework sheets meant for children could be made more colorful, with simpler words and characters to engage them. Therapists working with children find the need to be more creative to engage their clients while ensuring the skills are learnt effectively.
Though they may not appreciate cartoons or imaginative characters, delivery of CBT may have to be altered for adolescents. This would mainly depend on how well they are able to understand abstract concepts and how aware they are of their thoughts. Mostly, content and examples used have to be tailored to suit their age. For example, when asking to identify thoughts or feelings in a situation, therapists have to think of scenarios that a teen may face.
References
Yang, Z., Oathes, D. J., Linn, K. A., Bruce, S. E., Satterthwaite, T. D., Cook, P. A., Satchell, E. K., Shou, H., & Sheline, Y. I. (2018). Cognitive Behavioral Therapy Is Associated With Enhanced Cognitive Control Network Activity in Major Depression and Posttraumatic Stress Disorder. Biological psychiatry. Cognitive neuroscience and neuroimaging, 3(4), 311–319. https://doi.org/10.1016/j.bpsc.2017.12.006
Carpenter, J. K., Andrews, L. A., Witcraft, S. M., Powers, M. B., Smits, J., & Hofmann, S. G. (2018). Cognitive behavioral therapy for anxiety and related disorders: A meta-analysis of randomized placebo-controlled trials. Depression and anxiety, 35(6), 502–514. https://doi.org/10.1002/da.22728
Kodal, A., Fjermestad, K., Bjelland, I., Gjestad, R., Öst, L. G., Bjaastad, J. F., Haugland, B., Havik, O. E., Heiervang, E., & Wergeland, G. J. (2018). Long-term effectiveness of cognitive behavioral therapy for youth with anxiety disorders. Journal of anxiety disorders, 53, 58–67. https://doi.org/10.1016/j.janxdis.2017.11.003
Sprich, S. E., Safren, S. A., Finkelstein, D., Remmert, J. E., & Hammerness, P. (2016). A randomized controlled trial of cognitive behavioral therapy for ADHD in medication-treated adolescents. Journal of child psychology and psychiatry, and allied disciplines, 57(11), 1218–1226. https://doi.org/10.1111/jcpp.12549



